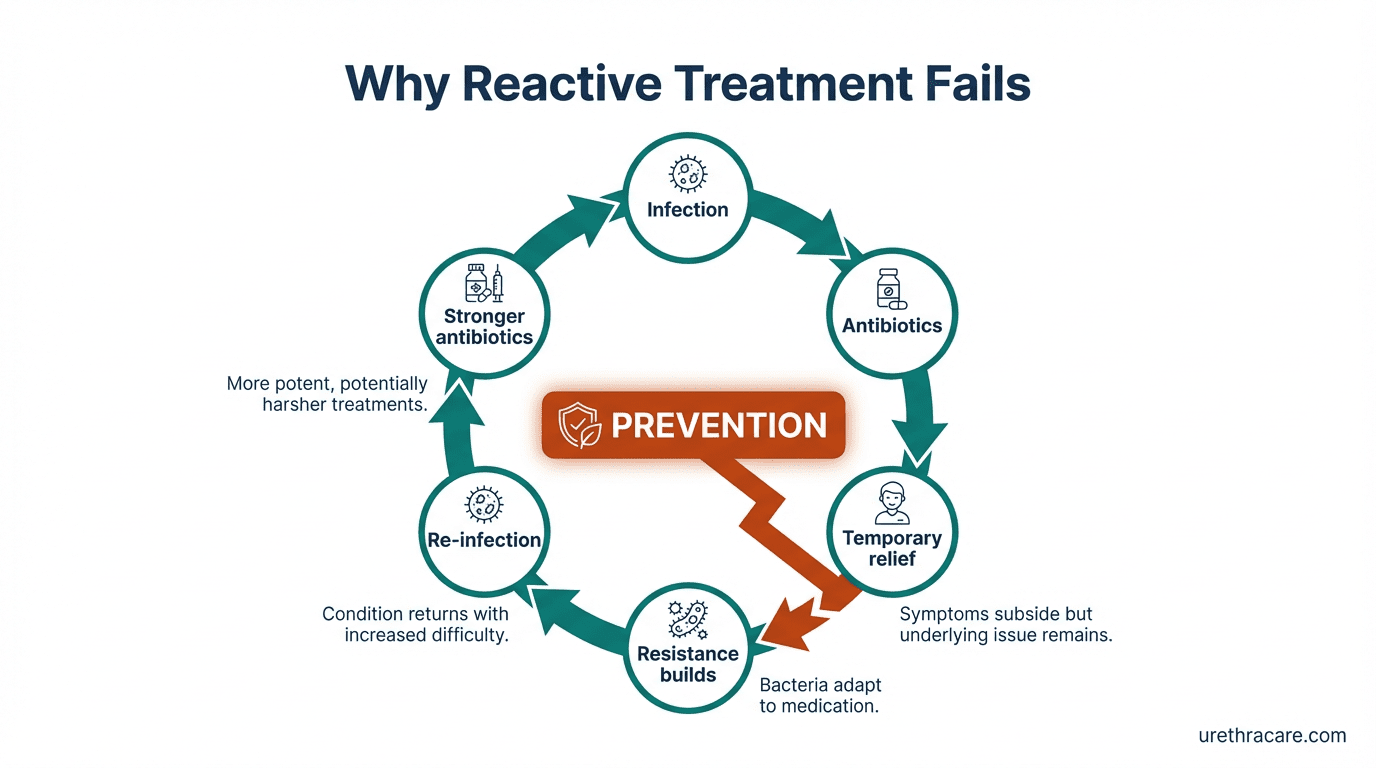
The Problem Isn't Antibiotics—It's How and When We Use Them
Urinary tract infections affect 50% of women in their lifetime. A 2024 study reveals that 16.7% of UTI treatments fail. But the headlines miss the real issue: the problem isn't that antibiotics don't work—it's that we're using systemic oral antibiotics reactively after bacteria have already established infection, instead of topical antimicrobials proactively at the source.
The Reactive Treatment Trap
A retrospective cohort study published in October 2024, analyzing US data from 2017-2022, found:
- 16.7% of female outpatients with uncomplicated UTIs experienced treatment failure
- Patients with prior treatment failure had even worse outcomes (33.9% failure rate)
- The average time to treatment failure was just 7.5 days
Why such high failure rates? By the time symptoms appear, bacteria have already ascended from the urethral opening, colonized the urinary tract, and established strongholds that systemic antibiotics struggle to eradicate.
The Ascending Infection Problem
Research increasingly confirms that urinary tract infections follow an ascending pattern—bacteria enter at the distal urethra and migrate upward. This has profound implications:
- The entry point is the urethral opening—exposed to external contamination
- Sexual activity can cause microtrauma and introduce or redistribute microbes
- Once bacteria ascend and establish themselves, they're far harder to eliminate
The current medical approach ignores this ascending nature. We wait for infection to establish, then prescribe systemic medications that must travel through the entire body to reach the infection site. It's like fighting a house fire by spraying water from a helicopter instead of using a hose at the source.
Topical vs. Systemic: A Critical Distinction
There's a fundamental difference between:
Systemic antibiotics (oral pills):
- Must be absorbed, distributed throughout the body
- Affect gut microbiome and beneficial bacteria
- Arrive at infection site diluted
- Used reactively, after infection established
Topical antimicrobials (local application):
- Applied directly at the entry point
- Minimal systemic absorption
- High concentration where it matters
- Can be used proactively, before infection takes hold
The oral hygiene analogy is instructive: we don't wait for tooth decay and then take antibiotic pills. We periodically reduce pathogenic microbial load through local measures—brushing, flossing, mouthwash. The same logic applies to urethral health.
The Statistics Support Prevention
The 2024 study identified high-risk groups with even worse treatment outcomes:
| Risk Factor | Treatment Failure Rate |
|---|---|
| Prior antibiotic failure | 33.9% |
| Recurrent UTI history | 21.1% |
| Age 75+ years | 20.9% |
Notice the pattern: recurrence breeds more recurrence. Each failed treatment makes the next infection more likely. Systemic antibiotics after the fact cannot break this cycle—but proactive, topical hygiene at the source might.
The Cost of Waiting
Patients experiencing treatment failure incur an average of $570 more in healthcare costs per episode. Multiply this across a lifetime of recurrent infections, and the financial burden becomes staggering.
More importantly, there's the toll on quality of life—the anxiety, the discomfort, the disruption of repeated infections and treatments.
A Different Approach: Prevention at the Source
The 2025 AUA/CUA/SUFU guidelines now emphasize prevention strategies over repeated treatment. But they stop short of the obvious conclusion: if infections ascend from the urethral opening, why not address microbial load there—with topical antimicrobials applied proactively?
We propose that using topical antimicrobial agents at key moments (such as during sexual activity) can reduce pathogenic microbial load before bacteria have a chance to ascend and establish infection.
The Bottom Line
The research is clear: treating UTIs with systemic antibiotics after they've established fails nearly 1 in 5 times. The answer isn't more powerful oral medications—it's smarter use of topical antimicrobials as a proactive hygiene measure, applied at the entry point before bacteria have a chance to ascend.
Prevention at the source. That's the paradigm shift we need.