They Named the Bacteria
For years, benign prostatic hyperplasia has often been explained as if it were simply the price of getting older: the prostate enlarges, symptoms appear, and treatment begins only after the process is already well underway. But a 2025 review in Frontiers in Oncology adds something critically important to the conversation: specific microbes associated with BPH severity.
That matters because it moves the story upstream. Instead of asking only why the prostate is inflamed, enlarged, and obstructive, we can ask the deeper question: what keeps provoking that inflammation in the first place?
The bacteria are no longer anonymous
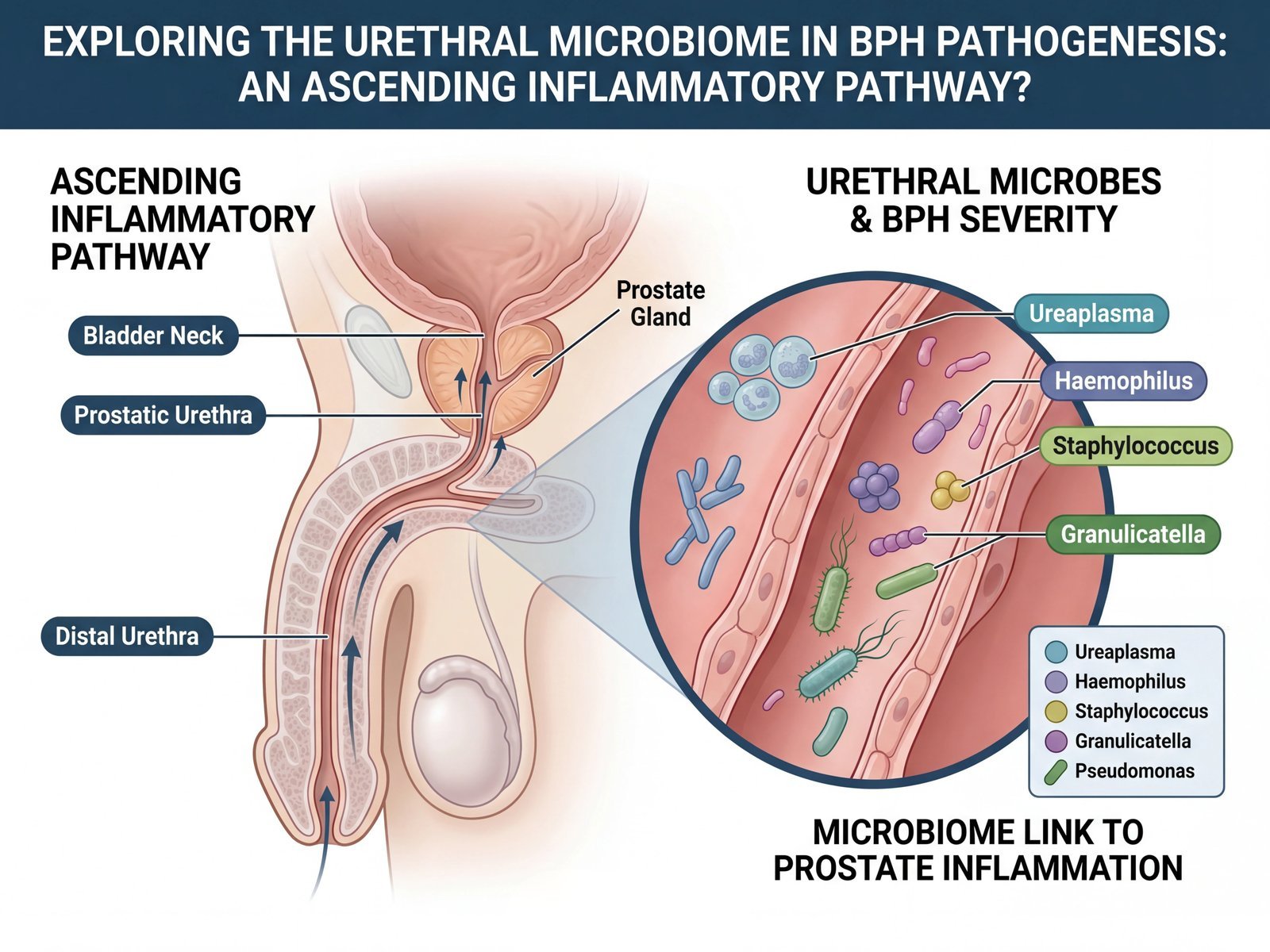
According to this review, organisms such as Ureaplasma urealyticum, Haemophilus, Staphylococcus, Granulicatella, Listeria, and Pseudomonas emerge as important microbial players in the BPH discussion. That does not mean every man with BPH has the same microbial profile, or that one single organism explains every case. But it does mean something highly significant: the old assumption that BPH is disconnected from microbiology is becoming increasingly difficult to defend.
In plain English, this review strengthens the idea that prostate enlargement may not arise out of nowhere. It may instead reflect a longer, quieter process involving urethral dysbiosis, chronic immune activation, and repeated inflammatory injury.
Why this finding strongly reinforces the Ascending Subclinical Urethritis model
The ASU model argues that low-grade urethral inflammation can persist quietly, recur repeatedly, and then ascend toward the prostatic urethra and prostate. This review does not prove every part of that model by itself. But it does something extremely important: it provides named microbial candidates and a plausible biological route from urethral dysbiosis to prostatic enlargement.
That is a major step forward. A theory based only on inflammation can be dismissed as too broad. A theory supported by inflammation and specific microbial associations becomes much harder to ignore.
From microbes to symptoms: the hidden chain reaction
Why would these organisms matter? Because microbes do not need to cause an obvious, acute infection to cause damage. Low-grade dysbiosis can continuously stimulate immune signaling, oxidative stress, and abnormal tissue responses. The review highlights pathways involving NF-kB activation, inflammatory cytokines, epithelial-mesenchymal transition, impaired apoptosis, and tissue remodeling. Those are not trivial findings. They describe exactly the kind of biology that can transform a healthy prostate into an enlarged, stiff, obstructive one over time.
- Step 1: The distal urethral environment becomes dysbiotic or chronically irritated.
- Step 2: Microbial products and host responses sustain low-grade inflammation.
- Step 3: Inflammatory signaling spreads upstream toward the prostatic urethra and prostate.
- Step 4: Cytokines and stress pathways promote hyperplasia, fibrosis, and abnormal remodeling.
- Step 5: The result is the familiar BPH picture: urinary symptoms, obstruction, and progression over time.
One especially important point from the review is the role of Pseudomonas-linked signaling in pathways tied to inflammation, cell survival, and structural change. That helps connect the microbiology to a believable disease mechanism, rather than leaving it as a vague association.
Why this matters clinically
If this line of evidence continues to hold up, then BPH should not be viewed only as an aging prostate that randomly enlarges. It should be viewed, at least in many men, as a condition that may be fed by persistent upstream inflammatory triggers. That changes the prevention conversation completely.
It suggests that protecting urethral health, reducing repeated inflammatory insult, and addressing hidden microbial imbalance earlier may be far more important than mainstream BPH care has historically acknowledged.
The bigger message
The most important takeaway from this paper is not simply that “bacteria exist.” It is that researchers are beginning to identify which bacteria, which pathways, and which mechanisms may connect chronic urethral inflammation to the structural changes seen in BPH.
That is precisely the kind of evidence a prevention-focused model has been waiting for.
For years, men have been told that prostate enlargement is just something that happens with age. Research like this points toward a different possibility: in many cases, the process may be inflammatory, microbial, and more preventable than we have been led to believe.
The prostate may not be the beginning of the story after all. It may very well be the urethra!