The Inflammation-BPH Connection: What New Research Reveals
For decades, benign prostatic hyperplasia (BPH) was considered an inevitable consequence of aging. But a surge of research in 2024 and 2025 is challenging this assumption, pointing to chronic inflammation as the primary driver of prostate enlargement.
The Statistics Are Staggering
- 50% of men in their 60s are affected by BPH
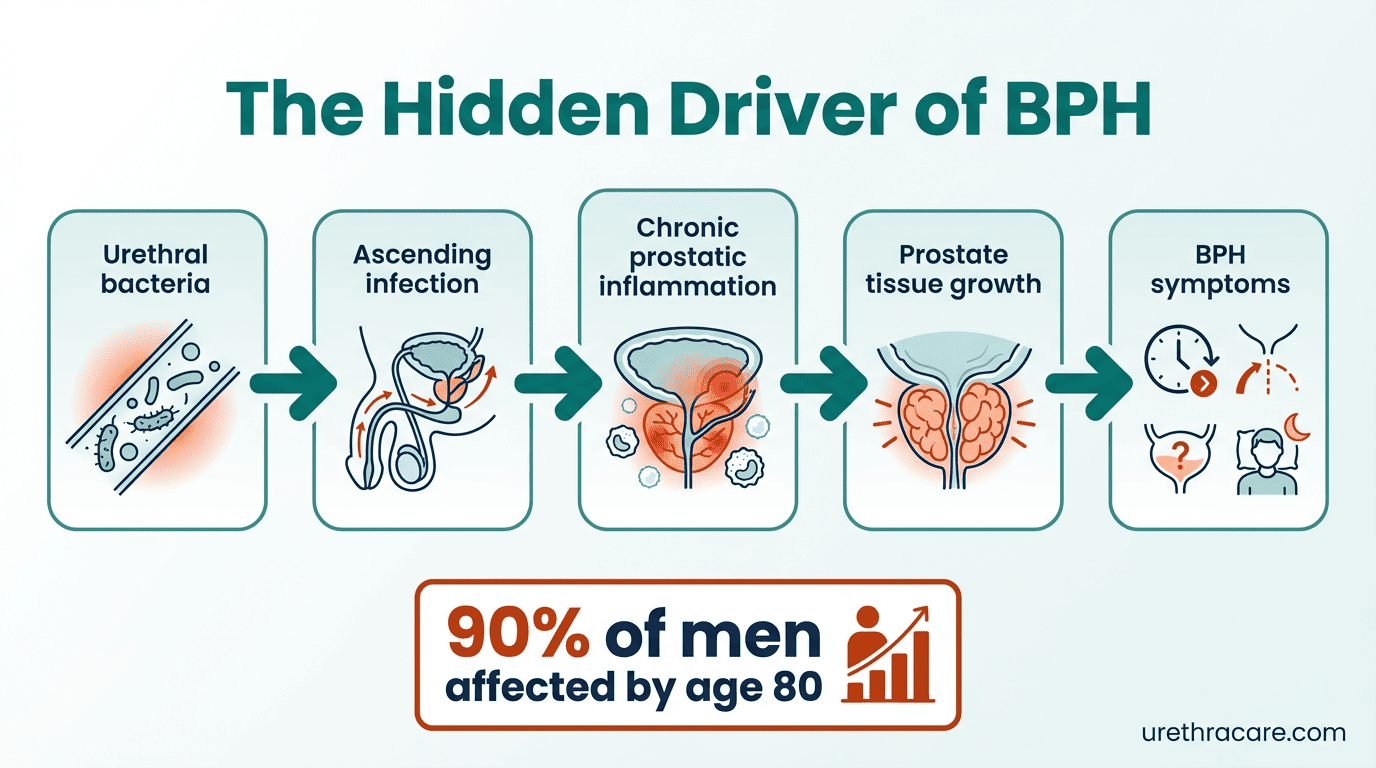
- 90% of men by age 80 will develop the condition
- The global urology devices market is projected to reach $48.6 billion by 2028
Yet despite these numbers, most treatments remain reactive rather than preventive.
What the Latest Research Shows
A comprehensive review published in the International Journal of Urology (June 2024) identified chronic prostatic inflammation as a key exacerbating factor in BPH. The research found that:
Inflammatory cytokines, particularly interleukin-17 (IL-17) and interleukin-8 (IL-8), play crucial roles in tissue remodeling and smooth muscle contraction within the prostate, thereby influencing BPH progression.
This aligns with findings from the American Journal of Clinical and Experimental Urology (2025), which demonstrated that:
- Inflammation drives collagen accumulation in the prostate
- This leads to tissue stiffening and urethral constriction
- The result: voiding dysfunction resembling human lower urinary tract symptoms (LUTS)
The Ascending Urethritis Hypothesis
What makes this research particularly significant is its alignment with the ascending urethritis hypothesis—the idea that chronic, low-grade inflammation originating in the urethra may ascend to the prostate, resulting in subclinical prostatitis that accumulates over time.
As research from StatPearls (2024) notes:
Most commonly, bacterial prostatitis results from an ascending infection from urethritis... In younger men, ascending urethral infection following anal or vaginal intercourse is a common pathology.
Why Prevention Matters
Patients with chronic prostatic inflammation often experience:
- More severe symptoms (LUTS)
- Resistance to conventional treatments
- Increased need for surgical intervention
The research points to a simple but revolutionary idea: what if we could prevent the inflammation before it starts?
Just as we brush our teeth daily to prevent oral disease, could proactive urogenital hygiene prevent the cascade of inflammation that leads to BPH?
The Bottom Line
The 2024-2025 research is clear: BPH is not simply "aging"—it's inflammation. And inflammation can potentially be prevented.
More time = More inflammatory events = More prostate growth.
This elegant understanding of BPH opens the door to prevention strategies that address root causes rather than just managing symptoms.